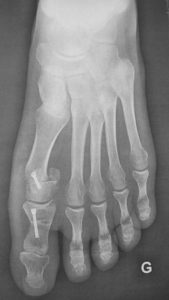
Definition
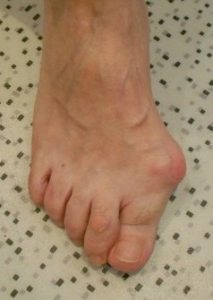
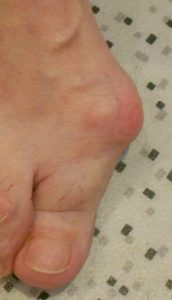
Hallux valgus is a forefoot deformation concerning the big toe (called hallux). It is deviated laterally towards the other toes and a “bump” appears on the medial side of the foot. It is commonly called “bunion”.
Causes
Many reasons can explain the onset of hallux valgus. Nevertheless, two of them are more frequent than the others.
Anatomical factors
The anatomy of the forefoot is one of the main elements to explain hallux valgus. It may occur when this anatomy changes from usual morphology:
- the length excess of the first metatarsal, which is more frequent patients with hallux valgus than without
- the deviation of the joint between first metatarsal and the big toe, which predisposes to the deviation of the hallux itself
- the “Egyptian” type of forefoot morphology, in which the big toe is longer than the 2nd
- the excess of mobility of the first metatarsal in its joint with this rest of the foot, which eases the deformation leading to the hallux valgus
However, “anatomical factors” doesn’t necessarily mean hereditary. The foot anatomy as it is at birth isn’t only the consequence of family genetic transmission (hereditary). The family background of hallux valgus, even numerous, are not an absolute proof of a hereditary disease. Mechanical explanations are also frequent.
Acquired mechanical factors : the shoes
The shoes act like an external element imposing a constraint on the big toe. Whatever the design is, they deviate the hallux towards the other toes, especially the “pointed-tip” ones.
The heels are also concerned since the higher they are, the more they bring the foot forward, precisely where the shoe is the tightest.
Other mechanical factors may ease the onset of the deformity but their responsibility is controversial: weight excess and flat foot. In both cases, the explanation would be the increase of mechanical stress on the foot and the first metatarsal.
Patients concerned
Women
Women represent the vast majority of patients. This firstly reflects their hormonal impregnation, increasing ligaments laxity. As we have seen, it fosters the hallux valgus onset by allowing an excess of mobility of the entire first ray.
On the other hand, women are culturally more concerned by wearing hight heels and “pointed-tip” shoes. Therefore, with same anatomical constitution as men, they are more prone to develop a hallux valgus.
Age
Two large profiles of patients consult for a hallux valgus :
- young patients, around 25-30 years old, mostly suffering from a congenital deformation
- older patients, around 45-50 years old and over, more often suffering from a acquired hallux valgus, in who the mechanical stress was acting through time on their foot and led to the deformity
Consequences on the daily life
The only presence of a big toe deformation isn’t enough to consider it as a pathology. It is all the tough work for the surgeon to recognize when the patient crosses the limits of a normal state. Identifying the daily consequences is therefore mandatory.
Big toe pain
Pain is the key symptom of hallux valgus. Pain is located on the big toe especially when using the foot intensively. For instance at the beginning of hallux valgus, long lasting hiking tracks, sports in a standing position or jumping, or simply daily walk when the disease has progressed. Normally, the pain decreases when stopping the effort, but it can occur even at night.
When it is present every day, it engenders overwhelming difficulties for the footwear. Sometimes, it even has consequences on the patient’s social life, for example when renouncing to the simplest activity needing to wear shoes.
Bursitis
The bone protrusion at the medial aspect of the foot is in conflict with the shoe. When the conflict lasts, a red and hot “inflammatory” zone appears. Very painful at the slightest contact it’s called bursitis when filled with liquid. In the most evolved cases, the bursitis tears and a viscous content poors out. The risk of deep infection comes when skin germs take advantage of the opening to colonize the cavity.
In some cases, pain isn’t limited to the big toe. Hallux valgus unloads mechanically the first metatarsal head and overloads the other metatarsal heads (called lateral rays). Callus, sometimes very spread and thick, appears on the plantar skin facing these bones as a reaction to overload. This may generate pain under the forefoot, sometimes more important than pain from hallux valgus.
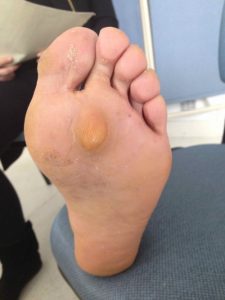
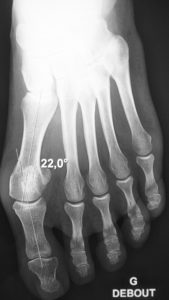
Hallux valgus : an important deformity may affect the lateral rays. Here, the 2nd metatarsal receives an excess of stress, reflected by the callus
Pain and bursitis put aside, patients meet important difficulties to footwear. The triangular shape of the forefoot makes it incompatible with the majority of usual models. Less and less shoe models are compatible, not only regarding the shape but also the heel’s height with high heels becoming impossible to wear.
Forefoot is at the convergence of two issues. The first is functional and the consequences of hallux valgus described above makes the foot incompatible with a normal function, that’s to say with no limit nor pain.
The second one is esthetic: the choice of “showcase” shoes or simply shoes enhancing the visual aspect of the foot.
Without ignoring the esthetic dimension, it is important to remember that orthopaedic surgery aims to restore a functional foot. A purely esthetic request cannot alone lead to surgery.
Avoid surgery
Choosing the shoes
To make the foot bearable everyday, the patient heads his choices to adapted designs. The “pointed-tip” models are incompatible with the foot width. They are to be proscribed.
High heels increase the mechanical forces under the forefoot. Their height must be limited to 3cm to reduce the load.
Finally, shoes composed with flexible materials are preferred to lower the expression of the conflict with the bone “bump”. Also, models where seams are in contact with the “bump” should be avoided. These seams make the shoe’s fabric or leather hyper-rigid, worsening the conflict with the hallux valgus.
Orthotic insoles
Orthotic insoles can decrease load on the big toe’s joint and thus relieve pain, likewise for the lateral metatarsals, where the can distributes load among metatarsal heads.
However, they reduce the available space in the shoe, and can major the conflict with the internal bone “bump”.
Sometimes, they are indispensable to correct severe abnormalities of the foot’s architecture, like severe flat feet. Without orthotics in these cases, hallux valgus surgery is exposed to an important risk of failure or recurrence.
Surgical decision
Surgery is an option only after the failure of simple and less agressive treatments.
Decisional criteria
Among all the consequences of the hallux valgus enounced above, none is to be considered more than another. Only one parameter is relevant to make a decision: the daily handicap. Shall it be professional, social or personal, it sums up the functional state of the patient’s foot.
When he consults, the patient is awaiting the surgeon to take a decision. And he would simply have to stick to it. However, only the patient shall evaluate the handicap he expresses.
No-surgery criteria
In some situations, the surgeon has to know how to take the decision not to perform surgery.
Preventive surgery
Preventive surgery shall not be accepted even if a hallux valgus may worsen with time. A foot without functional symptom is a foot whose architecture fits with the function. A surgical procedure will transform this bony architecture and may generate pain.
Very rare situations are an exception to the rule. For example, diabetes is a chronic disease that is likely to engender serious foot complications. For these patients prevention is mandatory and preventive surgery lowers the global risk.
“Plastic surgery” of the foot
Bone surgery of the foot is a major procedure whose aggressiveness cannot serve an esthetic aim as they are more likely to be are source of patient’s dissatisfaction. His eye and the surgeon’s have a different look on the deformity and a result may displease to one and satisfy the other if assessed on the only esthetic criteria.
An isolated esthetic criteria must not be considered alone. Nevertheless, we shouldn’t ignore it and preserve it as far as possible, if surgery happens for good reasons.
Unreasonable expectations
The expected results of surgery must be clearly exposed by the surgeon. He has to make sure the patient pursues realistic aims, particularly concerning pain and footwear.
The patient’s postoperative dissatisfaction is often the consequence of a difference between what he expected and the actual result. The surgeon’s role, before surgery, is to confront the patient to the future probable realities, and not let him think wrongly that all his wishes will come true.
“Will I wear heels again? Would I wear them all day or only for an evening?”. Depending on the case, the answer can whether be “yes” or “never”. The surgeon has to make the patient understand in advance, what seems possible to him, without ever losing sight the principle goal: have a functional foot, that is to say walking without pain.
Surgical techniques of the hallux valgus
Correction basics
Many procedure are described to correct a hallux valgus. They all respond to the same correction basics. They aim to correct the deformities to restore harmonious mechanical constraints on the forefoot.
One of the pillars of modern hallux valgus surgery are the osteotomies. They are bone cuts performed by the surgeon to reorient the axis of the foot. They allow first metatarsal straightening and erase bone protrusion.
“Soft tissues” section or lengthening can be associated. Over-the-years retracted tendons, ligaments and joint envelopes are thereby addressed.
If the correction basics are very precise, they might be performed according to various techniques. For instance osteotomies can be realised with a motorised saw, with bone scissors, or with a rotative burr.
The patient is thus facing a complex surgical context, involving techniques and surgical principles in which he gets lost.
Despite all the possible variants obeying all to the same mechanical principles mentioned above, two families of techniques seem to prevail. They respond to the same basics, but differ by the way the surgeon accesses to the bone and the soft tissues.
The classical « open » surgery
This method is the eldest and probably still the most widespread. The surgeon accesses largely to the anatomic structures he wants to correct. Cutaneous incisions are large enough to ensure a direct visual control on every step of the procedure.
This type of surgery is considered by their partisans as the most complete for the capacity of resolving all the patient’s problems, but also more precise in its execution under the visual control.
The osteotomies in open surgery are mostly of the “scarf” type or “chevron” type. To fix the bones in their new orientation, hardware is implanted : screws, staples, wires. The most often they are not necessarily to be removed as these implants are buried deep in the bone and perfectly well tolerated.
Percutaneous surgery
This surgical modality has been imported in France and Europe via Spain in the early 2000, coming from the US. It consists in accessing bone and soft tissues through millimetric incisions. The correction basics are the same, only the implementation modality is different.
It requires dedicated instruments, specifically developed to burr the bone protrusion, cut the bone, and perform the sections of soft tissues. Of course, the direct visual control is missing, since everything is realized through very small holes. Therefore, it is replaced by a low-irradiation peroperative radiography, called fluoroscopy.
Another particularity of these techniques is the possibility not to implant fixation hardware. It is replaced by a bandage made by the surgeon with great care at the end of surgery.
Sometimes, this procedure is considered as innovative because the operation time is shorten, the price is lower since no material is implanted, and it’s performed under local anaesthesia.
The immediate postoperative management is easier because the surgical aggressiveness is decreased. Patients are seduced by the “marketing” effect of an outpatient procedure with low pain and reduced scars.
However, despite an apparent harmlessness, this type of surgery is particularly difficult to perform. It is reserved for operators specifically formed and trained.
Combined minimally invasive and percutaneous surgery
The fast development of percutaneous surgery is certainly based on the major improvement of the postoperative period explained by a lower surgical aggressiveness.
However, specific complications linked to this technique modality have been identified after a few years of followup. Prudence is needed compared to classical open surgery where all steps are better controlled.
Nevertheless, inspired by this lower surgical aggressiveness coming from the percutaneous surgery, open procedures have been adapted to reach a reasonable compromise: the minimally invasive surgery. Incision is shorten as far as possible to reduce aggressiveness, but is kept long enough to ensure a visual control, missing in percutaneous surgery.
Moreover bone corrections are made stable with hardware fixation (screws) instead of a bandage, allowing immediate full weight-bearing on the operated zone.
Finally, when percutaneous procedures are possible without the compromise of their reliability, they remain purely percutaneous.